Gastroshiza is a rare congenital medical condition that affects how a baby’s abdominal wall forms during early pregnancy. In gastroshiza, the abdominal wall does not close fully, allowing the intestines and sometimes other organs to develop outside the baby’s body. This condition is present at birth and requires immediate medical care.
Although the medical community more commonly uses the term gastroschisis, many people search online for gastroshiza. For clarity and search optimization, this article uses the keyword gastroshiza while also explaining its relationship to the medically accepted term. Understanding gastroshiza is important for parents, caregivers, and anyone seeking reliable health information written in clear and simple language.
What Is Gastroshiza?
Gastroshiza is a birth condition where a baby is born with an opening in the abdominal wall, usually on the right side of the belly button. Through this opening, the intestines come out and are exposed to the amniotic fluid during pregnancy.
Unlike some other abdominal wall defects, gastroshiza does not usually involve a protective membrane covering the organs. This direct exposure can cause swelling, irritation, and damage to the intestines before birth.
Key features of gastroshiza include:
- A small opening in the abdominal wall
- Intestines located outside the body
- No protective sac covering the organs
- Immediate need for surgical treatment after birth
Gastroshiza is considered rare, but its reported cases have increased over the past few decades, especially among younger mothers.
How Gastroshiza Develops During Pregnancy
Early Fetal Development
During normal fetal development, the intestines temporarily move outside the abdomen and later return inside as the abdominal wall closes. In gastroshiza, this closure does not happen completely.
Doctors believe gastroshiza develops very early in pregnancy, often within the first month. The exact reason for this failure is not fully known, but research suggests it may involve blood flow problems or issues with how the abdominal wall tissues form.
Possible Biological Mechanisms
One leading theory is that a disruption in blood supply weakens part of the abdominal wall. When this area fails to develop properly, an opening forms. Through this opening, the intestines extend outside the body.
This explanation helps researchers understand why gastroshiza usually appears in the same location and why it often occurs without other major birth defects.
Also Read: Glaadvoice Com: A Complete and Updated Guide to the Platform Shaping Inclusive Media Culture
Gastroshiza vs Other Abdominal Wall Defects
Many people confuse gastroshiza with other conditions. Understanding the differences helps families and patients better understand the diagnosis.
Gastroshiza vs Omphalocele
Gastroshiza:
- Organs are outside the body without a protective sac
- Opening is usually small and off to the side of the belly button
- Less likely to be associated with genetic conditions
Omphalocele:
- Organs are covered by a thin membrane
- Opening is centered at the belly button
- More often linked with chromosomal or genetic conditions
This distinction is important because it affects treatment plans and long-term outcomes.
Risk Factors Associated With Gastroshiza
While gastroshiza can happen in any pregnancy, research has identified several risk factors that increase the likelihood.
Maternal Age
One of the strongest known risk factors is young maternal age. Teen mothers and women in their early twenties have a higher risk compared to older mothers. The reason for this is still being studied.
Lifestyle and Environmental Factors
Studies suggest that certain exposures during early pregnancy may raise the risk of gastroshiza:
- Smoking
- Alcohol use
- Use of recreational drugs
- Poor nutrition
- Limited access to prenatal care
These factors may affect blood flow or tissue development in the early embryo.
Socioeconomic Considerations
Lower access to healthcare and nutrition may indirectly increase risk. This highlights the importance of early and consistent prenatal care.
How Gastroshiza Is Diagnosed
Prenatal Diagnosis
Most cases of gastroshiza are diagnosed during pregnancy through routine ultrasound. Doctors can often see the intestines floating outside the baby’s abdomen.
Blood tests may also show elevated levels of alpha-fetoprotein, which can signal an abdominal wall defect.
Early diagnosis allows healthcare teams to:
- Monitor fetal growth
- Plan the delivery
- Arrange immediate surgical care after birth
Diagnosis at Birth
If gastroshiza is not detected during pregnancy, it is immediately visible at birth. The exposed intestines are obvious, and the baby is quickly transferred to specialized care.
Monitoring Pregnancy With Gastroshiza
Once gastroshiza is diagnosed, the pregnancy is considered high risk. However, many babies with gastroshiza are born healthy with proper care.
Regular Ultrasounds
Doctors use frequent ultrasounds to check:
- Intestinal condition
- Fetal growth
- Amniotic fluid levels
This monitoring helps determine the best time and method for delivery.
Delivery Planning
Most babies with gastroshiza are delivered in hospitals with neonatal intensive care units. Vaginal delivery is often possible, but some cases may require a cesarean section depending on the baby’s condition.
Immediate Care After Birth
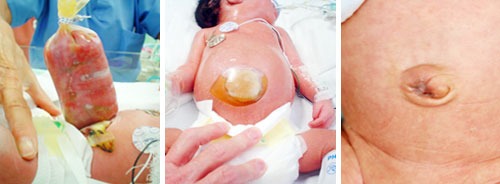
Protecting the Organs
After birth, the exposed intestines are carefully protected to prevent infection, dehydration, and heat loss. This is usually done with sterile coverings.
Also Read: Phoebe Cates Net Worth: A Deep Look at Her Wealth, Career, and Smart Life Choices
Stabilization
Before surgery, doctors focus on:
- Keeping the baby warm
- Providing fluids
- Preventing infection
- Supporting breathing if needed
This stabilization phase is critical for successful treatment.
Surgical Treatment Options for Gastroshiza
Surgery is required for all babies born with gastroshiza. The approach depends on how much intestine is outside the body and the baby’s overall condition.
Primary Closure Surgery
If the opening is small and the intestines are not too swollen, surgeons may place the organs back into the abdomen and close the opening in one operation.
This approach often leads to faster recovery but is not suitable for all cases.
Staged Repair With a Silo
When the intestines are very swollen or there is limited space in the abdomen, surgeons use a silo. A silo is a sterile pouch placed over the intestines.
Over several days, the organs are gently guided back into the abdomen. Once they are fully inside, the opening is closed surgically.
Recovery in the Neonatal Intensive Care Unit
Babies with gastroshiza usually spend several weeks in the NICU.
Feeding Challenges
The intestines need time to heal and start working properly. During this time:
- Babies receive nutrition through intravenous feeding
- Breast milk or formula is slowly introduced
- Feeding progress is closely monitored
Infection Prevention
Because gastroshiza involves exposed organs and surgery, infection prevention is a top priority. Strict hygiene and careful monitoring are essential.
Long-Term Outcomes for Children With Gastroshiza
Survival Rates
With modern medical care, survival rates for gastroshiza are very high, often above 90 percent in developed healthcare systems.
Digestive Health
Some children may experience:
- Slow digestion
- Feeding intolerance
- Occasional bowel issues
Most of these problems improve over time with proper medical follow-up.
Growth and Development
The majority of children with gastroshiza grow up to lead normal, healthy lives. Early developmental support can help address any delays related to long hospital stays.
Living With a Gastroshiza Diagnosis as a Family
Emotional Impact
A gastroshiza diagnosis can be overwhelming. Parents often experience fear, guilt, and anxiety. These feelings are normal and valid.
Support from healthcare teams, counselors, and other families can make a significant difference.
Also Read: Prostavive Colibrim: A Complete, Easy-to-Read Guide for Prostate and Urinary Health
Parental Involvement
Parents play a key role in recovery by:
- Learning about care routines
- Participating in feeding plans
- Advocating for their child’s needs
Advances in Gastroshiza Research and Care
Ongoing research continues to improve outcomes for babies with gastroshiza.
Prenatal Care Improvements
Better imaging and monitoring allow doctors to detect complications earlier and adjust care plans accordingly.
Surgical Innovations
Less invasive techniques and improved materials have reduced recovery times and complications.
Nutrition and Gut Health Research
Researchers are exploring ways to support intestinal healing and function, including specialized feeding strategies.
Prevention and Risk Reduction
There is no guaranteed way to prevent gastroshiza, but certain steps may reduce risk:
- Early prenatal care
- Avoiding smoking and alcohol
- Maintaining good nutrition
- Managing chronic health conditions
Public health efforts focused on education and access to care may help lower rates over time.
Common Myths About Gastroshiza
Myth: Gastroshiza Is Caused by Something the Parent Did
There is no single cause of gastroshiza. Parents should not blame themselves.
Myth: Children With Gastroshiza Cannot Live Normal Lives
Most children recover well and live full, active lives.
Myth: Gastroshiza Is Always Life-Threatening
While serious, gastroshiza is highly treatable with modern medical care.
Why Accurate Information About Gastroshiza Matters
Misinformation can increase fear and confusion. Reliable, easy-to-read content helps families:
- Make informed decisions
- Communicate effectively with doctors
- Feel empowered during treatment
By focusing on clarity and accuracy, this article aims to serve as a trusted resource.
Frequently Asked Questions About Gastroshiza
Can gastroshiza be missed during pregnancy?
Yes, although most cases are detected by ultrasound, some may not be identified until birth, especially if prenatal care is limited.
Does gastroshiza affect future pregnancies?
Having one child with gastroshiza slightly increases the risk in future pregnancies, but the overall risk remains low.
Is long-term medication required for children with gastroshiza?
Most children do not need long-term medication. Some may require temporary digestive support during early childhood.
Can adults who were born with gastroshiza have children?
Yes, adults born with gastroshiza can have children. There is no strong evidence of a high inheritance risk.
Are there support groups for families dealing with gastroshiza?
Yes, many hospitals and online communities offer support groups where families can share experiences and advice.
How long does intestinal healing usually take?
Healing time varies, but many babies begin feeding normally within weeks to months after surgery.
Is breastfeeding possible for babies with gastroshiza?
Breast milk is often encouraged because it supports digestion and immune health, even if feeding starts slowly.
Final Thoughts on Gastroshiza
Gastroshiza is a serious but manageable condition. With early diagnosis, skilled surgical care, and ongoing support, most children affected by gastroshiza go on to live healthy and fulfilling lives.
Understanding gastroshiza empowers families and caregivers to navigate the journey with confidence. Clear information, compassionate care, and continued research are the foundation of better outcomes now and in the future.